Last updated: 11 March 2026
Sources and references What is prostate cancer?
Prostate cancer begins when abnormal cells in the prostate start growing in an uncontrolled way.
The prostate
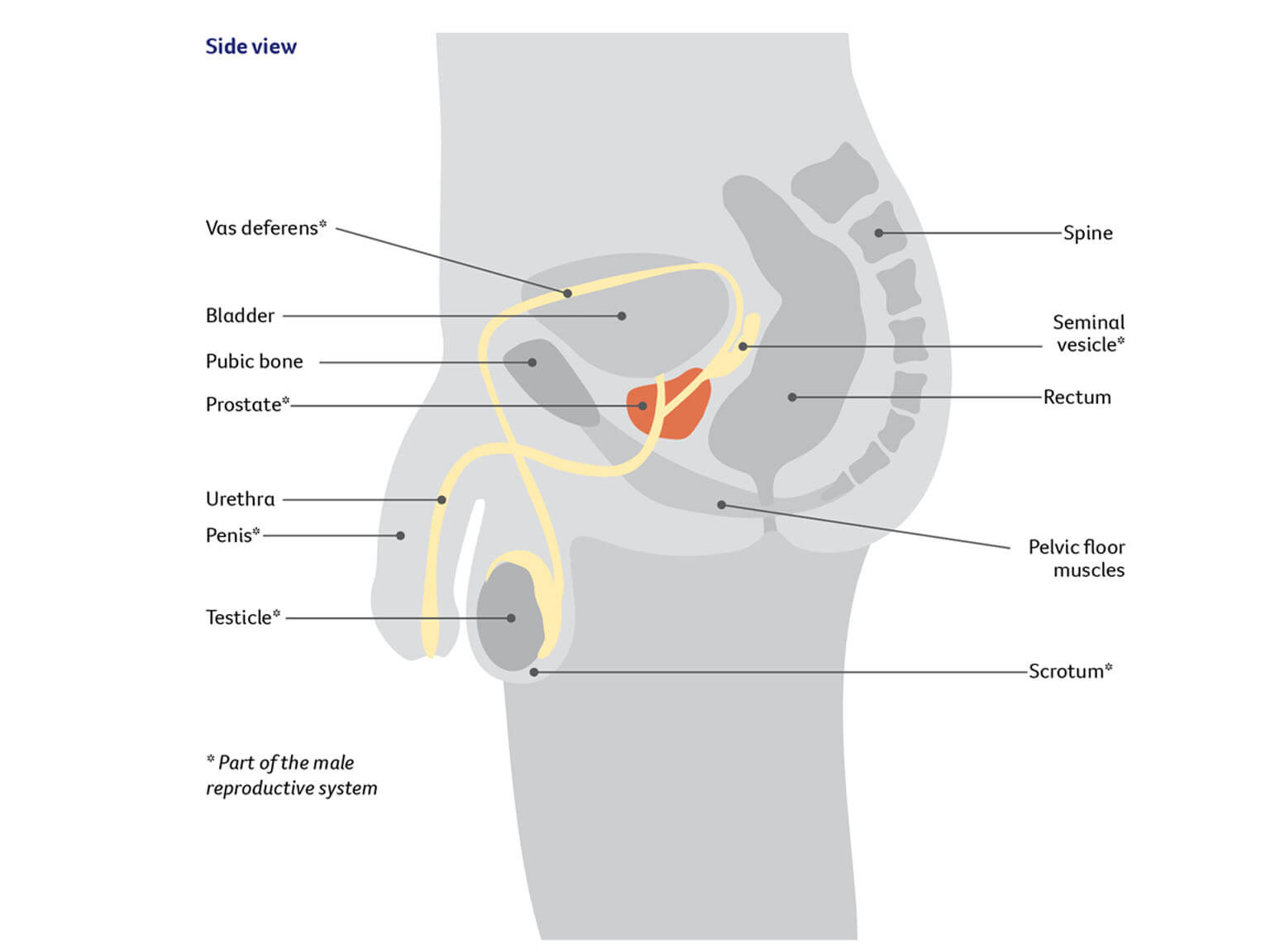
The prostate is a small gland about the size of a walnut. It forms part of the male reproductive system. The prostate sits below the bladder and in front of the rectum (the end section of the large bowel). Two glands called the seminal vesicles attach to the back of the prostate. The prostate is close to nerves, blood vessels, and muscles that help control erections and urination (the pelvic floor and urinary sphincter).
What the prostate does
The prostate produces fluid that helps to nourish and protect sperm. This fluid forms part of semen. Semen also contains sperm made in the testicles (testes) and fluid made by the seminal vesicles.
Urethra
This is a narrow tube that runs from the bladder and through the prostate to take urine (wee or pee) out of the body. The urethra also carries semen during ejaculation.
Ejaculation
When an orgasm occurs, millions of sperm from the testicles move through 2 tubes near the prostate called the vas deferens. The sperm then join with the fluids produced by the prostate and seminal vesicles to make semen. The muscle around the prostate contracts and pushes the semen into the urethra and out through the penis.
How the prostate grows
The main male sex hormone, testosterone, is made by the testicles and controls how the prostate grows. It is normal for the prostate to become larger with age. This may lead to a condition known as benign prostate hyperplasia or BPH.
How common is prostate cancer
Prostate cancer is the most common cancer in Australian men (except for skin cancer). About 1 in 12 men will get prostate cancer by the age of 70, and 1 in 5 will get it in their lifetime.4 About 25,500 men are diagnosed each year, and rates are increasing. This may be in part because the population is growing and people may be living longer.
Anyone with a prostate can get prostate cancer – men, transgender women and intersex people. For information specific to you, speak to your doctor.
Does prostate cancer run in families?
Having a strong family history of cancer increases the risk of developing prostate cancer. You may have inherited a gene that increases your risk of prostate cancer if you have:
- several close relatives on the same side of the family (can be your mother’s or father’s side) with prostate, breast and/or ovarian cancer, especially if due to a fault in the BRCA1 or BRCA2 genes
- a brother or father diagnosed with prostate cancer before the age of 60. In this case your risk is twice that of others.
If you are worried about your family history, talk to your general practitioner (GP). They may refer you to a family cancer clinic.
For more information, call Cancer Council 13 11 20.
Sources and references
This content has been developed by Cancer Council NSW on behalf of all other state and territory Cancer Councils as part of a National Cancer Information Subcommittee initiative. We thank the reviewers: Prof Declan Murphy, Consultant Urologist, Director – Genitourinary Oncology, Peter MacCallum Cancer Centre and The University of Melbourne, VIC; Alan Barlee, Consumer; Dr Patrick Bowden, Radiation Oncologist, Epworth Hospital, Richmond, VIC; Bob Carnaby, Consumer; Dr Megan Crumbaker, Medical Oncologist, St Vincent’s Hospital Sydney, NSW; Henry McGregor, Health Physiotherapist, Adelaide Men’s Health Physio, SA; Jessica Medd, Senior Clinical Psychologist, Department of Urology, Concord Repatriation General Hospital and Headway Health, NSW; Dr Gary Morrison, Shine a Light (LGBTQIA+ Cancer Support Group); Caitriona Nienaber, 13 11 20 Consultant, Cancer Council WA; Graham Rees, Consumer; Kerry Santoro, Prostate Cancer Specialist Nurse Consultant, Southern Adelaide Local Health Network, SA; Prof Phillip Stricker, Chairman, Department of Urology, St Vincent’s Private Hospital, NSW; Dr Sylvia van Dyk, Brachytherapy Lead, Peter MacCallum Cancer Centre, VIC. We also thank the health professionals, consumers and editorial teams who have worked on previous editions of this title
Cancer Council 13 11 20
Call us to talk to a specially trained health professional for free and confidential support and information.
Guide to best cancer care
This prostate cancer guide explains the standard of high-quality cancer care that all Australians can expect, from diagnosis, to treatment, recovery, and living with cancer.



